Treatment for Long Haulers Syndrome (October 2023)
The survey’s results mean that over 18 million adult Americans are currently experiencing symptoms of long COVID and 15 million have problems performing daily activities because of it.
The presence of spike protein has been strongly linked with long COVID. Studies have shown that spike proteins are often present in symptomatic patients, sometimes even months after infections.
As we learn more about post-COVID syndrome, however, the definition has been refined to be more accurate and useful:
- Subacute or ongoing COVID-19 (post-acute COVID-19 syndrome): symptoms continuing beyond four weeks from acute infection, up to 12 weeks.
- Post-acute sequelae of COVID-19 (PASC): symptoms persisting beyond the four weeks after acute infection.
- Post-COVID-19 syndrome (long COVID, long-hauler’s syndrome): chronic ongoing COVID-19 symptoms beyond 12 weeks from acute infection.
In this Article:
- Symptoms of Long Haulers Syndrome
- FLCCC I-Recover Protocol
- Diet and Nutrition
- Intermittent fasting
- Exercise
- Post-Vaccination Long Haulers?
- COVID Spike Protein Treatment for Kids
Symptoms of Long Haulers Syndrome
- Long COVID
- Post-acute COVID-19
- Long-term effects of COVID
- Post-acute COVID syndrome
- Chronic COVID
- Long-haul COVID
- Late sequelae
- Post-acute sequelae of SARS-COV-2 infection (PASC)
An international study showed that fatigue is the most common long-hauler’s syndrome, affecting 80% of all patients. Post-exertional malaise affects 73%, cognitive dysfunction affects 58%, sensorimotor symptoms such as loss of smell affect 56%, headache affects 54%, and memory issues affect 51% (R). A year after infection, common persistent symptoms include fatigue (reported by 82% of patients), brain fog (written by 67%), and headache (reported by 60%) (R).
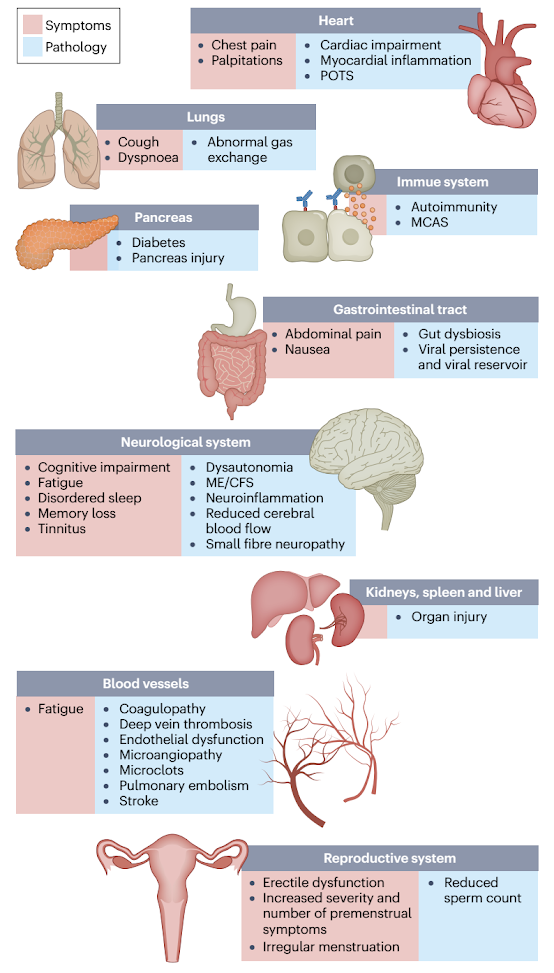 |
| Source: Davis, H.E., McCorkell, L., Vogel, J.M. et al. Long COVID: major findings, mechanisms and recommendations. Nature Rev Microbiol (2023) |
If the symptoms include major shortness of breath, cough with blood in it or pain on one side when you take a deep breath, it could be due to a late pulmonary embolism or a blood clot going to the lungs. Please visit your medical doctor or the nearest 24-hr medical emergency center immediately.
FLCCC I-Recover Protocol for Long Covid
The FLCCC (Front Line COVID-19 Critical Care Alliance) was formed by leading critical care specialists in March 2020, at the beginning of the Coronavirus pandemic, dedicated to developing highly effective treatment protocols to prevent the transmission of COVID-19 and to improve the outcomes for patients ill with the disease.Patients with post-vaccine syndrome should do whatever they can to prevent themselves from getting COVID-19. This may include a preventative protocol (see I-PREVENT) or early treatment in the event you do contract the virus or suspect infection (see I-CARE). COVID-19 will likely exacerbate the symptoms of vaccine injury.
Once a patient has shown improvement, the various interventions should be reduced or stopped one at a time. A less intensive maintenance approach is then suggested.
The core problem in post-vaccine syndrome is long-lasting “immune dysregulation.” The most important treatment goal is to help the body restore a healthy immune system — in other words, to let the body heal itself. Our recommended treatment strategy involves two major approaches:
- Promote autophagy to help rid the cells of the spike protein
- Use interventions that limit the toxicity/pathogenicity of the spike protein
Diagnostic Tests for Long COVID
The following basic tests are recommended — tests such as cytokines and chemokines, autoantibodies, and toxicological studies are expensive, have very little clinical relevance, and only complicate the management of long COVID patients.
- CBC with lymphocyte count and CD8+ count
- Chemistry with liver function tests
- CRP (inflammation)
- Ferritin (macrophage activation)
- D-dimer
- Early morning cortisol
- Thyroid function tests
- HbA1C—long COVID patients are at an increased risk of developing diabetes
- Autoantibodies: antiphospholipid antibody and ANA
- In patients with allergic features or those who experienced an acute reaction to the vaccine, the following tests may be helpful: eosinophil count; IgE levels, RAST testing and/or skin testing. Serum tryptase, serum histamine and/or 24-h urine N- methylhistamine should be considered in MCAS.
- Reactivated viruses: Antibodies/PCR against EBV Herpes I/II and CMV
- Vitamin D level
Specific Phenotypic tests
- CXR / chest CT with contrast
- Brain MRI
- ECHO
FIRST-LINE THERAPIES
(Not symptom specific; listed in order of importance; see full treatment strategy for detailed dosing information)
- Intermittent daily fasting or periodic daily fasts: Fasting stimulates the clearing of damaged mitochondria (mitophagy), misfolded and foreign proteins, and damaged cells (autophagy). Autophagy likely removes spike protein and misfolded proteins induced by the spike protein. Autophagy may therefore play a critical role in reversing the “spikopathy” induced by COVID infection. Indeed, activation of autophagy may be the only mechanism to remove intracellular spike protein.
- Ivermectin: It is likely that ivermectin and intermittent fasting act synergistically to rid the body of the spike protein. Ivermectin binds to the spike protein, aiding in the elimination by the host. Ivermectin also has potent anti-inflammatory properties.
- Moderating physical activity: Patients with long COVID frequently suffer from severe post-exertional fatigue and/or worsening of symptoms with exercise. We recommend moderating activity to tolerable levels that do not worsen symptoms, keeping the patient’s heart rate under 110 BPM. Furthermore, patients need to identify the activity level beyond which their symptoms worsen, and then aim to stay below that level of activity. Stretching and low-level resistance exercises are preferred over aerobic exercises.
- Low-dose naltrexone: This medication has been demonstrated to have anti-inflammatory, analgesic, and neuromodulating properties.
- Nattokinase: This highly effective fibrinolytic and antiplatelet agent targets the abnormal clotting that can occur from spike protein-related disease. (McCullough 2023)
- Melatonin: A powerful regulator of mitochondrial function, melatonin has anti-inflammatory and antioxidant properties. Should be taken prior to bedtime.
- Magnesium: At least 11 different types of magnesium are available, with varying bioavailability.
- Low-dose Methylene Blue: This is a therapeutic option in patients with brain fog and other neurological symptoms. The optimal dose is highly individualized and each patient needs to find the right dose for them.
- Sunlight and Photobiomodulation (PBM): Sunlight has great therapeutic powers. We suggest patients expose themselves to about 30 minutes of midday sunshine whenever possible (at least 3 times a week). A brisk midday walk is a viable alternative, as is red and NIR radiation emitted from LED panels.
- Vitamin D and K2
- Resveratrol or a combination flavonoid
- Probiotics/prebiotics: Patients with long COVID classically have a severe dysbiosis with loss of Bifidobacterium.
SECOND-LINE/ADJUNCTIVE THERAPIES
(Listed in order of importance; see full treatment strategy for detailed dosing information)
- Omega-3 fatty acids: We suggest a combination of EPA/DHA.
- N-acetyl cysteine (NAC): NAC has a broad range of antioxidant, anti-inflammatory, and immune-modulating mechanisms.
- Cardio MiracleTM and L-arginine/L-citrulline supplements: These supplements increase nitric oxide (NO) production.
- Nigella sativa: Taken as a supplement, in oil form, or as seeds, nigella sativa (also known as Black Seed or Kalonji) has antibacterial, antifungal, antiviral, anti-inflammatory, antioxidant, and immunomodulatory properties.
- Sildenafil with or without L-arginine-L-Citrulline: This may be helpful for brain fog as well as microvascular disease with clotting and poor perfusion.
- Bromelain: In vitro studies have demonstrated that bromelain cleaves the spike protein. This effect may be enhanced by NAC.
- Vitamin C: This vitamin is essential to human health and has important anti-inflammatory, antioxidant, and immune-enhancing properties. Oral Vitamin C also helps promote the growth of protective bacterial populations in the microbiome.
- Spermidine: Spermidine is a naturally occurring polyamine that, like resveratrol, has anti-inflammatory and antioxidant properties.
- Non-invasive brain stimulation (NIBS): Using transcranial direct current stimulation or transcranial magnetic stimulation, NIBS has been demonstrated to improve cognitive function in patients with long COVID as well as other neurological diseases.
- Intravenous Vitamin C
- Behavioral modification, relaxation therapy, mindfulness therapy
THIRD-LINE THERAPIES
- Hyperbaric oxygen therapy
- Low Magnitude Mechanical Stimulation
- “Mitochondrial energy optimizer”
- Hydroxychloroquine
- Low dose corticosteroid
A note about anesthesia and surgery:
Patients should notify their anesthesia team if using the following medications and/or nutraceuticals, as they can increase the risk of Serotonin syndrome with opioid administration:
- Methylene blue
- Curcumin
- Nigella Sativa
- Selective Serotonin Reuptake Inhibitors (SSRIs)
About Ivermectin
Ivermectin is a well-known, FDA-approved drug that has been used successfully around the world for more than four decades. One of the safest drugs known, it is on the WHO’s list of essential medicines, has been given over 3.7 billion times, and won the Nobel Prize for its global and historic impacts in eradicating endemic parasitic infections in many parts of the world.
Review the totality of supporting evidence for ivermectin: https://c19ivm.org.
It is likely that ivermectin and intermittent fasting act synergistically to rid the body of the spike protein.It appears that vaccine-injured patients can be grouped into two categories: i) ivermectin responders and ii) ivermectin non-responders. This distinction is important, as the latter are more difficult to treat and require more aggressive therapy.
For ivermectin responders, prolonged and chronic daily treatment is often necessary to support their recovery. In many, if the daily ivermectin is discontinued worsening symptoms often recur within days.
This protocol is solely for educational purposes regarding potentially beneficial therapies for COVID-19. Never disregard professional medical advice because of something you have read on our website and releases. This protocol is not intended to be a substitute for professional medical advice, diagnosis, or treatment with regard to any patient. Treatment for an individual patient should rely on the judgement of a physician or other qualified health provider. Always seek their advice with any questions you may have regarding your health or medical condition. Please note the FLCCC full disclaimer at: www.flccc.net/disclaimer
Be on the Lookout for Blood Clots for 90 Days
If you’ve had COVID-19, especially if it was a severe case, be aware that blood clots and heart problems, including heart attack, can occur for 90 days or more. It’s believed that remnants of the virus remain in the nervous system, the lungs, the heart and other organs.If the symptoms include major shortness of breath, cough with blood in it or pain on one side when you take a deep breath, it could be due to a late pulmonary embolism or a blood clot going to the lungs. “We’ve seen this on more than one occasion,” Dr Peter McCullough said.
Aside from a CT scan to rule out pulmonary embolism if you’re having symptoms and possibly a D-dimer test, McCullough suggests a high-sensitivity C-reactive protein (CRP) test, which provides a general index of inflammation. Keep in mind, though, as McCullough said:
“This pursuit of a blood clot is very important. I’ve seen multiple cases now where blood clots have been missed … this is now almost a daily occurrence, particularly within the first 90 days after COVID-19. I think after that period of time it becomes progressively less likely.”
Diet and Nutrition
It is believed that eating fruits, vegetables, and getting physical exercise is beneficial to thrombotic status—especially in those who are at risk of thrombotic diseases.
In many countries including the United States, recommendation for an antithrombotic diet and adequate physical exercise have been proposed by health authorities.
Supporting a good nutrient baseline is also key. “We see a significant amount of nutrient deficiencies and insufficiencies in the United States,” Boham says. Notably, insufficient levels of zinc and selenium are associated with worse outcomes from viral infections. Good sources of zinc include oysters, hemp seeds and pumpkinseeds, beans, nuts, and animal protein; sources of selenium include mushrooms, Brazil nuts, and seafood.
“Make sure you’re getting eight to 12 servings of phytonutrients a day from vegetables, fruits, spices, herbs, and tea,” she advises. Phytonutrients such as EGCG (epigallocatechin gallate, a polyphenol found in green tea) and curcumin (found in turmeric) can decrease inflammation and rebalance the immune system.
Antithrombotic Therapy (Ref)
In general, there are two classes of antithrombotic drugs: anticoagulants and antiplatelet drugs. Anticoagulants act on the clotting cascade and keep it from completion while antiplatelet medicines inhibit the platelets from activating and attaching to each other and the endothelium.Dr. Jordan Vaughn, internal medicine specialist in Birmingham, Alabama, says it’s key to start antithrombotic treatment in affected patients as early as possible.
“In the acutely ill from COVID-19, it was the sickest that I put on anticoagulation to prevent them from hospitalization. Starting them on DOAC and antiplatelet therapy was the foundation of keeping the hypoxic COVID-19 patient requiring hospitalization,” Dr. Vaughn said.
“After reading and understanding the COVID-19 associated coagulopathy, it was critical to understand this pathophysiology and manage this unique disease state because all of them are hypercoagulable. In acute severe COVID, I would treat patients with antithrombotic therapy and have them come back every few days to see if their symptoms improve.”
“In those that I would start anticoagulation, I started to notice that not only did they get better, but very few of them came back with long-term complications. So it seemed to me that, theoretically, it was like whatever we’re doing differently and treating these patients that are typically sicker was actually improving their symptoms in acute phase and also for the most part prevented the post-acute sequela that often came later in patients that were never acutely severe.”
Dr. Vaughn said he selects some coagulation lab tests to see if his patients were elevated in those factors at all.
“It was after the success of antiplatelet and anticoagulation in the acute treatment of COVID that I started to wonder about utilizing it in post acute sequelae COVID (PASC), and was led by diligent research to the work of Jaco Laubscher, Resia Pretorious, and Doug Kell.”
“It was as if a light bulb went off when I read their work. It profoundly changed how I look at both acute covid, but most importantly long COVID/PASC and their work was instrumental to truly helping suffering patients.”
Whether the cause of blood clots is the virus or vaccine, the symptoms do not differ much because the foundational cause is the spike protein.
Thus, when treating syndromes involving microclotting and local tissue hypoxia, regardless of the source of spike protein, the mess to clean up is the same.
It has been also reported that suitable and closely monitored “triple” anticoagulant therapy leads to the removal of the microclots and also removes symptoms.
It is a dual antiplatelet therapy (DAPT) (Ciopidogrel 75 mg and Aspirin 75 mg) once a day and direct oral anticoagulant (DOAC) (Apixiban 5 mg twice a day). In addition, it is important to include stomach protection with a medicine like a h2 blocker or a proton pump inhibitor.
At this point, the length of treatment is unknown and usually relies on a careful history of the patient’s interactions with the spike protein, time since last exposure, history of underlying autoimmune dysfunction, and overall functional symptomatology.
Dr. Vaughn’s treatments are driven by these factors, and typically lasts from one to three months. His hope is for a robust clinical trial soon to further inform length and identify additional surrogate clinical markers for clinicians to use to identify patients that would benefit from treatment.
Nutraceuticals for Thrombotic Conditions (Ref)
There are a variety of dietary supplements that may have a beneficial effect for thrombotic conditions (R).Meanwhile, many of these compounds also have anti-inflammatory, anti-oxidative, and autophagy-boosting effects which are beneficial for COVID-related symptoms as well.
Flavonoids
Resveratrol has antiplatelet properties. It is a naturally occurring flavonoid primarily found in grapes, red wine, and peanuts.
A dose-dependent inhibitory effect of resveratrol on platelet aggregation has been observed in cellular and animal models.
Furthermore, resveratrol’s multiple effects of lowering of oxidative stress and inflammation, enhancing metabolic capacity, increasing nitric oxide synthesis by endothelial cells, and promoting autophagy are beneficial for patients with COVID related clotting issues as well.
A major component in green tea, epigallocatechin-3 gallate (EGCG) is believed to actively inhibit platelets in humans. EGCG targets multiple pathways to achieve this role.
Genistein, a tyrosine kinase inhibitor, is an inhibitor of platelet aggregation and has effects in preventing thrombotic occlusion in blood vessels. It is found predominantly in soy products.
Genistein’s primary mechanism at least includes to inhibit platelet aggregation induced by collagen,; and antagonistic effects for thromboxane receptors.
Garlic
The compounds of adenosine, allicin, and paraffinic polysulfides appear to be responsible for the inhibitory effect of garlic on platelet aggregation.
Derived from the cleavage of alliin by alliin lyase, allicin inhibits platelet activity in vitro without affecting cyclooxygenase, lipoxygenase, thromboxane, vascular prostacyclin synthase, or cyclic AMP levels.
Antioxidants
Well known for its antioxidant function, vitamin E has multiple beneficial properties for clotting conditions.
For example, it improves the activity of endothelium-derived nitric oxide, improves endothelial function in part due to the inhibition of protein kinase C (PKC), and inhibits platelet aggregation.
Vitamin E has been shown to decrease platelet adhesion to collagen, fibrinogen, and fibronectin, and increase platelet sensitivity to prostaglandin E1.
Selenium is a trace element and an essential component of glutathione peroxidase enzymes, protecting cells from oxidative stress. A deficiency in selenium is associated with an increased risk of arterial thrombosis.
Selenium has an effect of inhibiting platelet aggregation, primarily through inhibiting those substances forming blood clots.
Drug Interactions
The impact of dietary supplements on normal hemostasis and antithrombotic therapy should be given consideration.
Supplements that have been reported to affect normal coagulation and platelet activity and/or have been reported to possibly interact with coumarin anticoagulants include danshen, garlic , ginkgo, American ginseng, Asian ginseng.
However, most of these reports are either theoretical or consist of individual cases.
Intermittent Fasting
Fasting also supports the turnover of damaged cells throughout the body, making room for new, healthy mitochondria and cells to take their place.
Time-restricted eating can take a variety of forms. One of the most popular is simply eating all your day’s meals within an eight-hour window, then going 16 hours without food or calories.
Exercise could help moderate the effects of Long COVID
COVID Jab Injuries Treatment for Kids
“If you're making spike [protein], even though kids don't have a lot of ACE2 receptors, those spikes are everywhere. In mice, it is shown that they cross the blood-brain barrier. They're disseminated, and then they tend to focus in your area of weakness.
They go into fat-loving tissues, they go into the ovaries, they seem to go everywhere. So, binding the spike protein, that's one aspect, and there are different things you can do, both pharmaceutical and non-pharmaceutical.
My favorite is ivermectin for the spike. I was giving kids 12 milligrams, initially, once a day. I went up to 12 mg twice a day for Omicron, but it depends on the size of the kid. For bigger kids, it’s 18 mg twice a day.
I didn't see any toxicity with ivermectin. I've used ivermectin before, mostly for parasitic infections, and I never had any problem with ivermectin. I have not used hydroxychloroquine before, but now, for Omicron, I would use hydroxychloroquine, 200 mg twice a day.
I use a lot of quercetin and zinc together ... To decrease inflammation, especially IL6, you also want to use a lot of immunomodulators, and a lot of supplements can do that.”
Moving Forward
- Find a Provider Directory
- List of Pharmacies that will fill Ivermectin
- www.ifm.org/find-a-practitioner (Functional Medicine)
- Post-COVID Care Centers (PCCC) by Survivor Corps
Z-Dtox Supplement
Your immune system can be weakened by over 300 different primary immunodeficiency disorders, poor diet, lack of sleep, and adverse reactions to various vaccines.
That’s where Z-DTOX comes in! Z-Dtox is Dr. Zelenko’s proprietary combination of NAC, EGCG, Zinc, Vitamin C, and Vitamin D.
Ingredients:
- Epigallocatechin gallate (EGCG) is an extract of green tea and is a powerful zinc Ionophore (zinc delivery system).
- N-acetyl cysteine (NAC) is a supplement form of cysteine. It may prevent blood clots and is an antioxidant.
- Zinc is critical for immune cell development. Dozens of different enzymes in the body rely on zinc.
- Vitamin C is an essential nutrient involved in the repair of tissue and the enzymatic production of certain neurotransmitters.
- Vitamin D is a group of fat-soluble secosteroids responsible for increasing intestinal absorption of calcium, magnesium, and phosphate, and many other biological effects.
Note: To get 5% OFF, please use this coupon code: drfrancis
- This post is not medical advice. This post is for informational and educational purposes only.
- Always see or talk to your doctor before taking these drugs, supplements and over the counter products. Be aware that most of the 'treatment' dosages are above the recommended dietary allowance (RDA) and therefore such dosages should not be maintained on a long term basis.
- Our aim here isn't to replace your doctors' advice. It is intended as a sharing of knowledge and information. Do take note that supplements are not 100% protective or curative against COVID-19.
- You still need to follow the advice given by CDC, WHO and your local authority in terms of local guidelines such as mask wearing, social distancing, vaccination and avoiding crowds. It's better to combine multiple strategies in order to defend yourself against this virus.
- According to US NIH: "...Guidelines should not be considered mandates. The choice of what to do or not to do for an individual patient is ultimately decided by the patient and their provider."
Related:



.png)





.png)

Comments
Post a Comment