Does Sugar Fuel Cancer? What the Science Actually Shows (2026 Update)
The statement “sugar feeds cancer” is widespread — but incomplete.
The relationship between sugar and cancer is not as simple as eliminating sugar to stop tumor growth. However, metabolic dysfunction, chronic hyperinsulinemia, and high glycemic load diets are increasingly recognized as contributors to cancer risk and possibly progression.
This article clarifies what we know — and what we don’t.
Sugars ‘Nourish’ Cancer Cells
 |
| Soft drinks on shelves in Riga, Latvia. Sugary drinks are prevalent across the world. (Tanya Keisha/Shutterstock) |
Cancer cells require a substantial amount of glucose to survive. In the 1930s, Otto Warburg, a German biochemist, discovered that both cancer cells and normal cells require sugar, but their metabolic pathways differ: Normal cells primarily convert glucose into energy through aerobic respiration, while cancer cells obtain energy through glycolysis instead of using oxygen.
Cancer cells produce very little and inefficient energy due to their unique method of metabolizing sugar, which is why they voraciously consume sugar—at a rate 200 times faster than normal cells. That appetite can have wide-ranging effects.
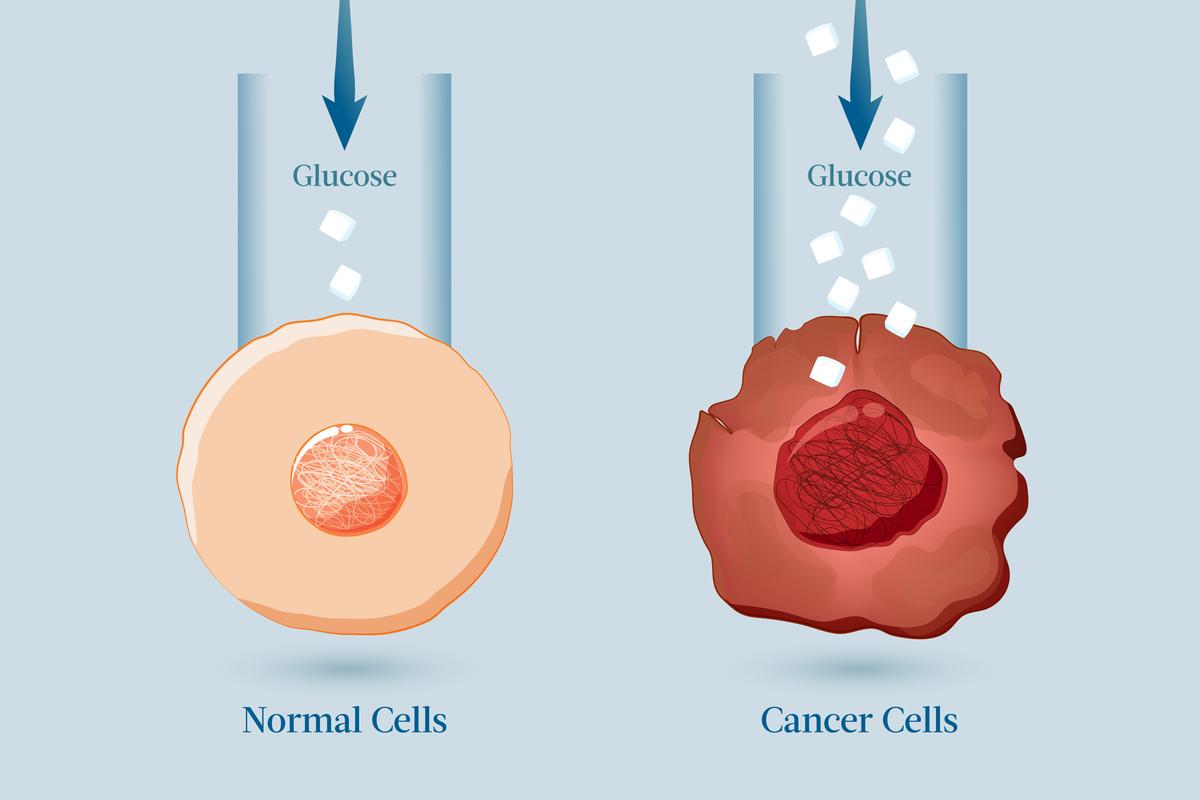 |
| Cancer cells consume sugar at a rate 200 times faster than normal cells. (Illustration by The Epoch Times, Shutterstock) |
“Cancer cells, in some sense, hijack metabolic processes in the body,” Lorenzo Cohen, professor and director of the integrative medicine program at MD Anderson Cancer Center and author of “Anticancer Living,” told The Epoch Times.
Sugar–Obesity–Cancer: A Prevailing Theory
A Challenging Problem
Nevertheless, prospective cohort studies—a type of observational study focused on following a particular group of people over a period of time without interfering with their eating habits—can provide valuable insights into the relationship between sugar intake and cancer risk.
This association remained significant even after adjusting for factors such as weight gain and body mass index. The study suggested that sugar may increase cancer risk through mechanisms other than just weight gain.
The Many Ways Sugar May Lead to Cancer
Processed sugar is a potent energy source. Beyond weight gain, it causes a variety of changes in your body that increase cancer risk.Alters Metabolism
“Another mechanism through which sugar increases the risk of cancer is its impact on metabolism,” Mr. Song said.High sugar intake can alter the metabolic profile, triggering inflammation and insulin resistance, both risk factors for tumor development.
This is a major mechanism that causes cancer, independently of obesity, he said. Obese people are more prone to inflammation and insulin resistance, but these can also occur in lean individuals.
Sucrose, fructose, and refined carbohydrates cause a significant spike in blood sugar levels. To maintain sugar balance, the body must increase insulin accordingly, and “excess amounts of increased insulin are inflammatory,” according to Mr. Cohen.
Triggers DNA Mutation
Inflammation and insulin resistance can also directly promote mutations in cell genes, leading to alteration in cell behavior.Mr. Song further explained that the normal cell life cycle is disrupted in such cases. Cells don’t undergo normal timely cell death, instead growing and proliferating without limits, fueling tumor development.
Affects Gut Microbiota
“Only in recent years have people started to recognize the significance of gut microbiota [in relation to cancer risk],” Mr. Song said.Sugar can disrupt the structure and function of gut microbiota and replace beneficial bacteria with harmful ones, ultimately resulting in the development of tumors in the intestines and even elsewhere.
Mr. Song explained several mechanisms by which the gut microbiome affects tumor development. These have also been a focus of recent research.
Sugar can increase certain harmful bacteria, which produce carcinogenic proteins on their surfaces, leading to gene mutations and directly promoting tumor development. Some harmful gut bacteria can also affect metabolism, causing uncontrolled cell growth.
Additionally, certain gut bacteria can harm the immune system, compromising its surveillance function. They may also produce specific metabolites that, upon entering the bloodstream from the gut, induce inflammation and immune dysregulation at distant sites, ultimately contributing to the development of tumors in those areas.
Undermines Immunity
Under normal circumstances, the immune system is responsible for clearing out problematic cells and maintaining a state of equilibrium. Overeating sugar for a prolonged period can disrupt this equilibrium, rendering the immune system unable to resist mutated cells or other pathways that promote cancer development.Generally, experts believe that sugar affects processes related to cancer, such as inflammation, glucose metabolism, lipid metabolism, and immune regulation. “I think obesity is just a byproduct [of these processes],” Mr. Cohen said.
According to Dr. Kortmansky, more extensive research is needed to better understand the potential pathways through which sugar might affect cancer.Fructose: The Most Dangerous Sugar
When we refer to “sugar” in general, we’re often talking about sucrose, Dr. Jason Fung, a nephrologist with a long-standing focus on Type 2 diabetes and intermittent fasting, told The Epoch Times.
A sucrose molecule consists of one glucose molecule and one fructose molecule. Every cell in the body can absorb glucose and use it as an energy source. However, fructose molecules aren’t used by any cells in the body. Instead, they enter the liver directly, where some are essentially converted into fat, leading to increased insulin resistance.
The researchers further discovered that among several diets based on sucrose, glucose, fructose, and a combination of glucose and fructose, the mice on the fructose-based diet exhibited the most severe conditions, with the highest breast cancer tumor weight and the most aggressive tumor growth. Cancer metastasis was also more common.
“Fructose and glucose are processed very differently in the body,” said Mr. Cohen, who was involved in the study. This experiment demonstrated that fructose directly promotes the growth of breast cancer.
High-fructose corn syrup, comprised of 45 percent glucose and 55 percent fructose, is frequently used in soft drinks and other sweetened foods.
Mr. Cantley, who led this study, said that in recent years, there was “a dramatic increase” in colorectal cancer among younger populations, which is associated with the sharp rise in how much high-fructose corn syrup people have started consuming over the past half-century.
The study from Spain mentioned earlier discovered that the consumption of liquid sugars is linked to a more significant increase in cancer risk than the consumption of solid sugars, especially liquid fructose and fructose in fruit juices. A high intake of liquid fructose was associated with the highest increase in cancer mortality.
Fructose in processed food and drinks differs from fructose in actual fruits. When eating an apple, you consume small quantities of fructose with fiber, slowing digestion.
But drinking an 8-ounce bottle of apple juice is like consuming the sugar from three to four apples all at once, Mr. Cohen said.
“I do recommend that people who are at risk focus on a diet that is low in added sugar and then a lifestyle that is high in physical activity,” Dr. Kortmansky told The Epoch Times. “That’s the best way to control the sugar that is in our system.”Steps That Reduce the Drivers of Cancer Risk
- Lower oxidative stress where it starts — Tobacco exposure directly drives the DNA damage pattern linked to stomach cancer, which makes complete avoidance essential. Energy balance matters just as much. Chronic carbohydrate restriction weakens mitochondrial energy production and increases reductive stress, which raises internal damage. Adequate carbohydrate intake — about 250 grams daily — keeps your cellular energy production running smoothly, like a well-tuned engine that produces power instead of smoke. When carbs are too low, your mitochondria struggle and sputter, creating the very oxidative stress you're trying to avoid.
- Minimize linoleic acid-rich seed oils to protect mitochondrial function — Inside each mitochondrion there’s a highly specialized structure called the inner mitochondrial membrane — the surface where energy production takes place. Roughly 20% of this membrane is composed of cardiolipin, a distinctive phospholipid that contains four fatty acid chains instead of the usual two. Keeping daily LA intake under 5 grams, and closer to 2 grams when possible, helps limit excess incorporation into these non-cardiolipin membrane compartments. This means minimizing seed oils hidden in packaged foods, sauces, dressings, and restaurant meals, and choosing more oxidation-resistant fats such as tallow, ghee, or grass fed butter.
- Remove habits that accelerate immune decline with age — Your immune system doesn't simply "get worse with age" — it changes, and certain habits accelerate its dysfunction. After 40, blood stem cell mutations become more common, but lifestyle factors determine whether these mutations dominate your immune system or remain in check. Alcohol undermines mitochondrial energy production and weakens immune signaling in your gut, which raises long-term risk. Protecting sleep timing and getting morning sunlight support circadian rhythm, the system that coordinates immune defense. A more responsive immune system clears damaged stomach cells before they accumulate additional mutations. Protect your circadian rhythm by maintaining consistent sleep/wake times within a 30-minute window, even on weekends. Get 10 to 15 minutes of outdoor morning sunlight within one hour of waking — no sunglasses — to set your circadian clock. Dim indoor lights after sunset and avoid screens in the hours before bed. Aim for sleep between 10 p.m. and 6 a.m. when immune repair functions peak.
Bottom Line
However:
Chronic excess refined sugar intake contributes to insulin resistance and hyperinsulinemia — metabolic conditions associated with increased cancer risk and possibly worse outcomes.
The clinically relevant target is:
Insulin signaling, body composition, and metabolic health.
In oncology, metabolic optimization supports systemic resilience — but does not replace standard treatment.
- Reduce ultra-processed foods
- Eliminate sugar-sweetened beverages
- Choose low glycemic index carbohydrates
- Increase fiber intake (≥30g daily)
- Pair carbohydrates with protein and healthy fats
- Engage in resistance training
Source and Reference:




.png)





.png)

Comments
Post a Comment