COVID-19 Death Rate: The Highest and the Lowest in the World (From Apr 2020 to Jul 2020)
It has been more than 2 months since we posted the article on COVID-19 death rate. Some articles said that doctors and scientists know more about COVID-19 now as compared to say 2 or 3 months ago. Does that translate into better outcomes such as the death rate? Let's compare the current death-rate vs the one in our previous article 2 months ago. Are we improving?
The COVID-19 death rate is defined as the the number of known deaths divided by the total number of confirmed cases – varies widely by country right now. We have selected countries that are among the highest and the lowest in the world.
Why is the Number important?
The number impacts how we determine our management. It's important to understand risk factors for severe outcome - so whether that differs by sex or the presence of other diseases, race, ethnicity, income status, hospital etc. This will allow the policymakers to identify groups that need more attention and intensive management.
Reference: https://coronavirus.jhu.edu/map.html
Read more: Coronavirus
COVID-19 is an emerging, rapidly evolving situation. Get the latest public health information from CDC: https://www.coronavirus.gov.
Get the latest research from NIH: https://www.nih.gov/coronavirus.
The COVID-19 death rate is defined as the the number of known deaths divided by the total number of confirmed cases – varies widely by country right now. We have selected countries that are among the highest and the lowest in the world.
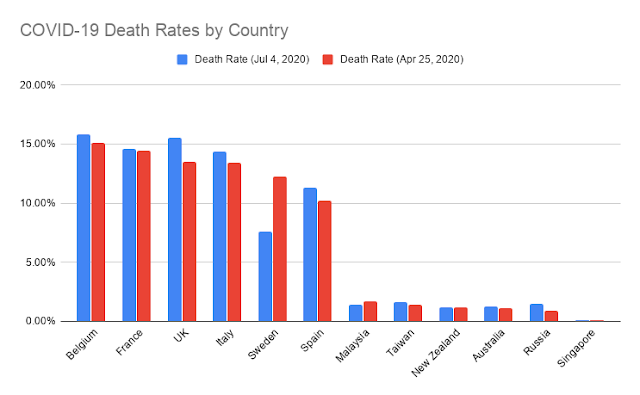 |
| COVID-19 Death Rates: Apr 25 vs Jul 4, 2020 |
As of Jul 4, 2020, the global death rate is at about 4.7%, a significant decrease as compared to 7% on Apr 25, 2020. This supports the theory that we are better at managing the disease, globally. Even 1% difference means a lot on a global scale.
That said, we have gone above 11 million confirmed cases worldwide and the number of new cases are getting scary for Brazil and US as shown in the chart below.
Daily confirmed new cases (5-day moving average): Outbreak evolution for the current 10 most affected countries
 |
| Credit: Johns Hopkins - last updated on Saturday, July 4, 2020 at 03:00 AM EDT |
As of Jul 4, 2020, Belgium is still among the highest in the world with a death rate at about 15%. Similarly high in France, United Kingdom and Italy; with not much improvement as compared to April 25, 2020.
An important highlight is Sweden, which has improved from 12.25% (Apr 25, 2020) to 7.6% (Jul 4, 2020) based on 'case fatality rate' (number of deaths vs total number of confirmed cases). However, in terms of per capita death rate (deaths per 100,000 population), Sweden is still among the highest.
Sweden's prime minister has ordered an inquiry into the failure of the country's no-lockdown coronavirus strategy. Unlike most other European countries, including its closest neighbours, Sweden did not implement strict, wholesale lockdown measures in response to the pandemic. Instead, the country has largely allowed businesses and hospitality to remain open and students to attend school.
The other end of the spectrum is Singapore, with a death rate of 0.1% (no change) even though the number of cases might have increased. Other Asia-Pacific countries such as Australia, Malaysia and Taiwan remain among the lowest in the world.
An important highlight is Sweden, which has improved from 12.25% (Apr 25, 2020) to 7.6% (Jul 4, 2020) based on 'case fatality rate' (number of deaths vs total number of confirmed cases). However, in terms of per capita death rate (deaths per 100,000 population), Sweden is still among the highest.
Sweden's prime minister has ordered an inquiry into the failure of the country's no-lockdown coronavirus strategy. Unlike most other European countries, including its closest neighbours, Sweden did not implement strict, wholesale lockdown measures in response to the pandemic. Instead, the country has largely allowed businesses and hospitality to remain open and students to attend school.
The other end of the spectrum is Singapore, with a death rate of 0.1% (no change) even though the number of cases might have increased. Other Asia-Pacific countries such as Australia, Malaysia and Taiwan remain among the lowest in the world.
Why the Variation among Countries?
An important point to note is that there are a lot of cases that are not confirmed. People who have mild illness might be turned away or not be able to access testing. And we also know that there are a lot of people who are infected but don't develop symptoms, so that means that there's actually a much bigger denominator than what is reflected in this 'death rate'.
High death rates could be the result of limited testing capacity. Countries with scarce testing resources tend to prioritise the most severe cases for COVID-19 confirmation, leaving many people with mild or asymptomatic cases undetected, thus giving the appearance of an unusually high death rate.
High death rates could be the result of limited testing capacity. Countries with scarce testing resources tend to prioritise the most severe cases for COVID-19 confirmation, leaving many people with mild or asymptomatic cases undetected, thus giving the appearance of an unusually high death rate.
Why is the Number important?
The number impacts how we determine our management. It's important to understand risk factors for severe outcome - so whether that differs by sex or the presence of other diseases, race, ethnicity, income status, hospital etc. This will allow the policymakers to identify groups that need more attention and intensive management.
We’ve all been hearing that the elderly and those with pre-existing conditions (JAMA) are more likely to get hit the hardest by COVID-19. In fact, a research study was just published out of New York that shows that in a large hospital system, COVID-19 patients that needed hospital care (JAMA):
- The average age was 63 with half of this group being age 52-75
- They were 60% male and 40% female
- 57% had high blood pressure
- 42% were obese
- 34% had diabetes
Conclusion
The global death rates are staying flat. The key is 'to keep the young people away from the old people,' according to Dr. Jeffrey Klausner, a professor of epidemiology at University of California, Los Angeles.
Major risk factors like high blood pressure, obesity, and diabetes can be modified or controlled and treated. If you have high blood pressure, a high fever will increase the blood pressure further. What does it mean? Your risk of heart attack and stroke will increase. If you suspect that you have COVID-19 or being exposed to someone with COVID-19, please consult your doctor as soon as possible, especially if you are in the high risk group.
The global death rates are staying flat. The key is 'to keep the young people away from the old people,' according to Dr. Jeffrey Klausner, a professor of epidemiology at University of California, Los Angeles.
Major risk factors like high blood pressure, obesity, and diabetes can be modified or controlled and treated. If you have high blood pressure, a high fever will increase the blood pressure further. What does it mean? Your risk of heart attack and stroke will increase. If you suspect that you have COVID-19 or being exposed to someone with COVID-19, please consult your doctor as soon as possible, especially if you are in the high risk group.
Reference: https://coronavirus.jhu.edu/map.html
Read more: Coronavirus
COVID-19 is an emerging, rapidly evolving situation. Get the latest public health information from CDC: https://www.coronavirus.gov.
Get the latest research from NIH: https://www.nih.gov/coronavirus.


.png)





.png)

Glad in our country, it is under control. Hope we go through this pandemic together well.
ReplyDelete