The Truth About Colonoscopies: Major Colonoscopy Study Reveals Surprising Result (Part 2)
As discussed in Part 1 of this series, colonoscopies are a major money-maker for the conventional medicine machine, generating at least $42B per year, year after year. Is it any wonder they backpedal on any suggestions that could reduce the number of annual procedures? The caveat is always ‘colonoscopies are the Gold Standard for screening’ (maybe it’s really just for the GOLD)? The cost of complications are not taken into consideration when analyzing the annual procedure fees.
I also briefly talked about polyps – which (surprisingly) rarely become cancerous. It should be no surprise that doctors can charge more for the procedure if they remove a tiny benign polyp.
We reviewed the risks of colonoscopies, including the REAL number of side effects and complications from this exam, especially when a polyp is removed. We discussed perforations, infections, and the importance of asking your doctor how many scopes s/he has done! The skill of the examiner is an independent risk factor for complications. We also reviewed the new study, published in October, 2022 in New England Journal of Medicine, that calls into doubt the need routine colonoscopies.
A conventional colonoscopy isn’t simply a routine doctor’s visit, but an ambulatory surgical procedure performed under anesthesia. The cancer industry has used its heavy-handed fear and propaganda machine to push tests that are costly, are not benign, may not be necessary and may not even lower the risk of cancer or death.
Here in Part 2, we will review other types of tests available to screen for colon cancer.
- Sigmoidoscopies – do you qualify?
- Testing stool for blood or cancer markers: Guaiac test, FIT test, Cologuard test
- Recent FDA-approved STOOL tests for colon cancer screening
- Various little-known BLOOD tests approved for colon cancer screening
- New tests under development
It makes sense to screen for colon cancer and if present, to identify and remove it at the earliest possible stage. An ideal screening test should be safe, readily available, convenient, inexpensive and have a high sensitivity. Screening colonoscopies are none of these!
Sigmoidoscopy
Screening methods for colon cancer are divided into invasive and non-invasive tests.
We’ve already discussed colonoscopy, an invasive test, with all of its risks. Another test, called a flexible sigmoidoscopy (FlexSig) is similar, except it less extensive. A FlexSig is faster (takes about 15 minutes), less complicated, and generally less expensive than colonoscopy. Intravenous sedation is usually not needed, and enemas are used for the preparation instead of the harsh oral preps used for several days prior to a colonoscopy. In addition, a colonoscope is about 66 inches long; a flexible sigmoidoscope is about 24 inches long and has a smaller diameter.
While flexible sigmoidoscopy can usually view the entire descending colon, other areas of the colon go unexamined. Therefore, there is a risk that cancers could go undetected if flexible sigmoidoscopy is undertaken alone.
To sort this out, a study was done in the UK (2018) to determine who can be screened using a FlexSig instead of undergoing a full colonoscopy.’
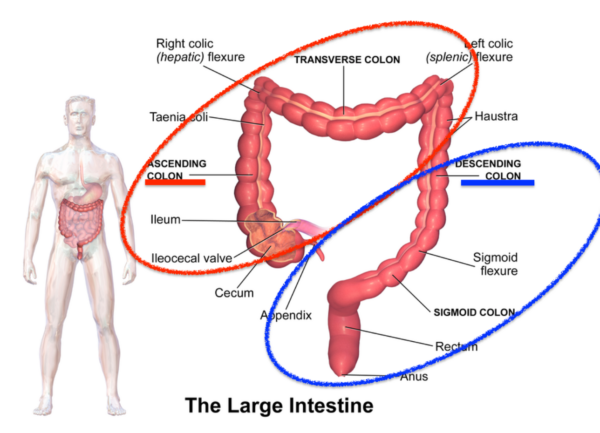
This is a multicenter study of 7,375 patients with suspected colon cancer who were referred from 21 hospitals throughout England. The study confirmed the strong association between anemia and abdominal mass with cancer in the ascending colon (cecum, ascending colon, transverse colon, splenic flexure – see above).
We found that 80% of descending colon cancers could be identified by using a broader definition of anemia [hemoglobin <11 g/dL men; <10 g/dL women]. If a narrower definition of anemia was used [hemoglobin <13 g/dL men; <12 g/dL women], only 39% of cancers were suspected and then identified.
Given the importance of anemia as a marker for colon cancer, we recommend all patients with suspected colon cancer have a full blood count.
This large study confirmed that ascending colon cancers are rare and found in less than 1% of patients without anemia and/or without abdominal mass. Patients who presented with only a change in bowel habits or with only rectal bleeding WITHOUT anemia rarely had colon cancer. Therefore, if the patient is not anemic, s/he is a good candidate for a sigmoidoscopy (FlexSig) for screening every 5 years plus annual fecal blood test instead of undergoing full colonoscopy every 10 years, unless it’s indicated for diagnostic purposes.
Non-Invasive Testing
Current screening methods for colon cancer are divided into invasive and non-invasive tests. Let’s look at the non-invasive screening tests.
Stool Test: Guaiac Fecal Occult Blood Test (gFOBT)
The least invasive and least expensive screening test for colon cancer is to check the stool for the presence of blood. Called a fecal occult blood test. (FOBT), this test has long been the most important ‘first step’ in the screening process for colon cancer. This simple test makes the most sense before immediately recommending colonoscopy for routine ‘screening’.
The guaiac fecal occult blood test (gFOBT) is used to identify blood in the stool that can’t be seen with the naked eye. Abnormal tissues or cancerous lesions are often fragile and can be brushed open as stool passes by, releasing tiny drops of blood.
The test involves placing a tiny amount of fecal matter on card coated with guaiac paper, a type of paper that contains the phenolic compound, alpha-guaiaconic acid, extracted from the wood resin of Guaiacum trees. Next, a small amount of hydrogen peroxide is dropped on the stool. If blood is present, the card yields a blue reaction product within seconds. The test is usually repeated on at least three different samples on different days, especially if the first test is negative because abnormal cells may not bleed all the time. The test should be done on a stool sample that is less than 24 hours old and can be done at home with a kit purchased from the drug store.
Guaiac tests are more sensitive for detecting blood from the lower than from the upper gastrointestinal tract because hemoglobin from red blood cells is degraded as it passes through the gastrointestinal tract. Keep in mind there conditions other than cancer that can release blood into the stool, such as inflammatory bowel disease, an ulcer or hemorrhoids. If this screening test is positive, additional diagnostic tests will be required.
While no prep is required to do the gFOBT, factors have been known to affect the results. It is advisable to avoid these medications and foods for 3 to 5 days before stool testing:
- Anti-inflammatory medications, such as Advil, Aleve, Ibuprofen, and aspirin
- Topical iodine preps
- Vitamin C and citrus fruits
- Red meat
While these avoidance recommendations have long been thought to give a more accurate test, a large Canadian meta-analysis (2010) evaluated this premise and concluded:
Most of the evidence evaluating the effect of dietary restrictions on FOBT results is outdated and of suboptimal quality. However, 4 RCTs and a meta-analysis of these data do not support dietary restrictions when screening for colorectal cancer.
Stool test: Fecal Immunohistochemistry Test (FIT)
In 2012, the World Endoscopy Organization Expert Working Group recommended FIT as a preferred technology for screening instead of gFOBT.
Similar to the guaiac stool test, the fecal immunochemical test (FIT)is used to identify non-visible blood in the stool. What makes FIT different is that it only detects human blood: it uses an antibody to human globin. There is no cross-reactivity with hemoglobin in dietary meats. Since medication and food do not interfere, the results are more accurate. FIT can accurately identify about 79% of colon cancers. Also, FIT is more specific for identifying blood from the colon. Test kids for home FIT tests are available online or at your local pharmacy.
Stool test: Cologuard, DNA testing
In August 2014,Cologuard® became the first DNA stool test approved by the FDA for colon cancer screening. Cologuard, manufactured by Exact Sciences, is approved for screening average-risk adults over 50 years old. Cologuard uses molecular tests to identify biomarkers and gene mutations related to colorectal cancer (for those who are research geeks, the markers tested for are KRAS mutation, BMP3, and NDRG4 methylation).
The sensitivity of a one-time screening with Cologuard test is 92% for colorectal cancer, but the sensitivity for advanced adenomas is around 50%. The downside to the Cologuard test is that it’s pricey: it costs between $450 and $700 and it is generally not covered by insurance. But compare that to the out-of-pocket cost of a colonoscopy AND the potential cost of its complications, this test really is a bargain!
Blood Tests for Colon Cancer
An observational study(2017) reported that 97% of subjects refusing colonoscopy accepted a non-invasive screening test. Of these 83% preferred a blood test. Here are two blood tests for colon cancer screening that are generally not suggested by your doctor!
Blood test: Epi proColon
Septins are a group of scaffolding proteins that provide structural support during cell division. Hypermethylated Septin9 DNAcan be found in the bloodstream as a tumor marker for colon cancer.
Epi proColon is a blood test – which can be obtained through LabCorp – can be used to detect the methylated septin 9 (mSEPT9) gene. Epi proColon is an FDA approved test for colorectal cancer screening. This simple blood test is able to detect a majority of colon cancer at all stages and all colorectal locations. The test should be obtained by individuals of average risk for colon cancer but who are unwilling or unable to undergo colonoscopy or a FlexSig exam.
It has been known since 2009 that the mSEPT9 blood test assay can successfully identify 72% of colon cancers with a specificity of 93% (in the training study) and identified 68% of colon cancers with a specificity of 89% (in the testing study.)
The test is reasonably price: Medicare payment rate for the test is $192. Some private insurers consider mSEPT9 to be investigational and may not pay for or reimburse the cost of the test. But again, given the challenges with invasive tests, this is an excellent option for non-invasive screening.
Blood test: Shield™ by Guardant Health
On May 2022,Guardant health announced the availability of Shield™, a blood test for the detection of early-stage colon cancer for asymptomatic individuals, 45yo and older.
The Shield assay demonstrated 91% sensitivity (detection rate) of colon cancer, including 90% for Stage I, 97% for Stage II, and 86% for Stage III colon cancer. The assay also demonstrated 20% sensitivity for advanced adenomas and 92% specificity (true negative rate) in normal cases. The test is not yet widely available, but read about it and ask your doctor to give you this option for screening.
On the Horizon
There are multiple modalities under development for alternative screening for colon cancer. I’ve listed a few here for general interest.
Colon capsule endoscopy
Examination of the colon via swallowing a pill, called a capsule endoscopy (CCE), allows minimally invasive assessment of the large bowel. This test has been under development since at least 2009.
Intensive bowel cleansing is required, in similar fashion to colonoscopy. Two meta-analyses of CCE showed this procedure had a sensitivity of 71% to 73% for detection of all polyps and a sensitivity of 68% to 69% for other ‘significant findings.’ While these findings are comparable to other noninvasive measures, the accuracy of the exam is largely dependent on the quality of the colon cleansing prep. The test has been shown to be well tolerated by patients. It is undergoing further research prior to release for general use.
circRNA biomarkers
Tumor markers are considered to be one of the best methods for the early detection of asymptomatic micro-focal tumors. Non-coding RNAs (ncRNAs) are a class of endogenous RNAs that are involved in the regulation of gene expression. Circular RNA (circRNA) is a type of ncRNA that can be manipulated into regulating many important biological processes.
circRNA has a high level of stability, making it a potentially valuable tumor marker for many type of cancers, including colon cancer. This research for colon cancer is in its infancy, but tissue biomarkers have long been used to follow treatment progress for several types of cancer.
Risk Factors
The risk factors for colon cancer, or any other form of cancer, can be divided into two categories: fixed and variable.
Fixed factors: things you CAN’T change:
- Age: The risk of colon cancer is higher in persons over 50 years old.
- Race: African-Americans are at higher risk of colon cancer.
- Genetic risks: Inherited syndromes are responsible for a small number of colon cancers.
- Family history of colon cancer: If you have a first degree family member who has had colon cancer, your risk is increased. First degree family member is a parent or a sibling. About 20% of all colorectal cancers are in persons who have a close relative with colorectal cancer.
- Personal history of advanced forms of inflammatory bowel conditions (Crohn’s disease, ulcerative colitis, etc).
- Personal history of many benign or cancerous polyps removed. This is evidence of an unhealthy colon so it increases the risk of progressing to full-blown cancer.
Genetic specialists estimate that between 5 and 10 in every 100 cancers (5 to 10%) diagnosed are linked to an inherited faulty or mutated gene. More than 75% of colon and rectal cancers occur in people with no known risk factors, which is why regular non-invasive, simple screening is important, as discussed in Part 3 of this series.
Epigenetics literally means ‘above genetics,’ suggesting there are factors that change the outcomes of our genes. Our DNA is not the sole determination of our health. Environmental pollutants, heavy metals, chronic viral and bacterial infections, hormone imbalances, physical and emotional stress, and most importantly, nutritional imbalances play a key roles in genetic expressions. This is good news; it means that just because you have a genetic mutation or family risk factor, it doesn’t mean that gene will ‘turn on’ and misbehave. Having a genetic marker for cancer is not a death sentence; there are things you can do to to travel a different road for health.
Variable and epigenetic factors you CAN change:
- Environmental pollutants. For several years now, we have been a big fan of Zeolite spray from Touchstone essentials to eliminate heavy metals and clear persistent organic pollutants (POPs) out of the body. To learn more about this Zeolite – and get a special discount for a first-time purchase – check out the information at this link.
- A sedentary lifestyle adversely affects the human body through various mechanisms. In fact, astudy from 2020 is an eye-opener on just how detrimental a lack of physical activity is to overall health. Sedentary behaviors increase all of the following: All-cause mortality, cardiovascular disease mortality, cancer risk, and risks of metabolic disorders such as diabetes mellitus, hypertension, and dyslipidemia; musculoskeletal disorders such as arthralgia and osteoporosis; depression and cognitive impairment. Therefore, increasing physical activity is important to promote both personal and public health. Twenty minutes of exercise every day can be life-changing.
- Being overweight by more than 20 pounds is an epigenetic risk factors for many adverse health conditions, including cancer.
- Dietary factors to embrace to lower the risk of colon cancer:
- Avoid high consumption of red and/or processed meat. Cooking meat at high temperatures can lead to the formation of mutagenic and carcinogenic compounds.
- Increase consumption of fresh fruits and vegetables.
- Drink at least 50% of your body weight in ounces per day of water. For example, if you weigh 200 lbs (90kg) you should be drinking close to 100oz of water per day.
All of this helps avoid constipation. As stool stagnates, the undigested food literally putrefies and rots. The longer stagnant stool remains in the body, the more acids are released that are toxic to the colon tissues and detrimental overall health. Having at least one large bowel movement per day is essential for a healthy body. Imagine if you filled your kitchen garbage disposal with left over food – and only flipped the switch once a week.
- Tobacco smoking. Just don’t do it – or stop. It’s a horrible toxin for all cells of your body.
- Alcohol consumption. Persons who consume an average of 2-4 alcoholic drinks per day have a 23% higher risk of colorectal cancer than those who consume less than one drink per day.
Keep Your Colon Healthy: Lab tests
One of the most important supplements to prevent cancer over all is Vitamin D. I recommend a level in the blood to be between 80-100 ng/ml.
You can get a full wellness panel PLUS vitamin D level – with over 50 individual laboratory tests screen for cardiovascular risk, major organ function, anemia, diabetes, infection, blood disease and other indications of illness – as part of this wellness panel. You can order also order lab tests from the comfort of your own home, without having to take time off from work to go to the doctor to just get an order to go to the lab. Order your tests here. We’ve been working with Direct Labs since 2004. You can trust them AND get your labs at a deep discount over using your insurance. If you have an HSA plan, perhaps you can turn in the cost of the tests for reimbursement.
Another assessment for the health of your colon is a stool test to assess the balance of biomarkers grouped into key areas relating to GI function:
- Maldigestion – do you have adequate digestive enzymes?
- Inflammation – do you have inflammatory markers?
- Dysbiosis – do you have an imbalance in your microbiome?
- Metabolite Imbalance – do you have inflammatory markers, such as calprotectin, EPX and sIgA in your gut?
- Infection – do you have an overgrowth of pathogenic bacteria generally not tested for in ‘ova and parasite’ routine screening?
There are several labs that do this type of advanced testing but Cyrex, Genova and Doctors Data are the three I am most familiar with. They all have advanced tests you can order and do at home. They also offer phone consultations to help with interpretation and recommendations.
Keep Your Colon Healthy: Food
The best basic foods for a health GI tract are fresh fruits, a healthy portion of raw or lightly steamed vegetables, beans, whole grains (preferably gluten-free options) and healthy fats, such as avocados, olives, and both olive and coconut oil.
You may also be able to prevent polyps by increasing your intake of vitamin D and calcium. Foods that are rich in vitamin D and calcium include:
- broccoli
- yogurt, milk, cheese – sources of vitamin D
- fish, eggs, poultry: Fish and poultry are alternative sources of protein and have been shown to reduce the risk of colon cancer and adenoma. Good fish choices are salmon, swordfish, white fish, and clean tuna.
Most of the time, it’s not possible to get enough vitamin D solely from food. Years ago, vitamin D deficiencies were rare when people rolled up their sleeves and worked outside from sun-up to sun-down. But as work shifted from farms to offices, that changed. Because pigmentation can reduce vitamin D production in the skin by over 90%, black and hispanic populations are at particular risk of vitamin D deficiency.
Vitamin K is another fat-soluble vitamin that exists in two forms: vitamin K1 (phylloquinone, mainly found in green leafy vegetables) and vitamin K2 (menaquinone, primarily found in fermented dairy.)
They work together synergistically: Vitamin D3 directs the absorption of calcium from your intestines into the blood. Vitamin K2 takes it from there, directing that calcium into your bones.
I advise that an optimal level of 25-hydroxyvitamin D should be between 80-100 ng/mL. Most people need to take between 2,000-10,000 IU (50 mcg-250 mcg) daily to achieve and sustain this level.
For vitamin K, current research has found high 180 μg/day resulted in improved clinical results compared to lower-dose supplementation. Opti Vitamin D3+K2 provides 180 mcg of MenaQ7® PRO, the most widely studied form of vitamin K2. Some people need more depending on the status of their bone and arterial health. If you’re not sure where you stand, ask your doctor to order a blood test for both 25-OH Vitamin D and Vitamin K or order the tests from home (except if you live in New York) through DirectLabs and this link.
Fermented foods
Fermentation is one of the most ancient methods of food preparation in the world. It is defined as a ‘technology in which the growth and metabolic activities of microorganisms are used to preserve foods.’ Fermentation also increases the shelf life of foods, especially highly perishable foods, so it is a preferred way for food storage in developing countries.
Food fermentation can be complicated and can loosely be divided into two categories: aerobic fermentation, and anaerobic fermentation. During fermentation, microorganisms are used to synthesize vitamins and minerals, produce biologically active peptides, and remove some toxins.
Biologically active peptides are also well known for their health benefits. Among these peptides, conjugated linoleic acids (CLA) have a blood pressure lowering effect, bacteriocins show antimicrobial effects, sphingolipids have anti-carcinogenic and anti-microbial properties. Bioactive peptides also exhibit antioxidant, anti-microbial, anti-fungal, anti-inflammatory, and anti-allergenic effects. The most common fermented foods include kefir, sauerkraut, natto, kombucha, kimchi and miso. This paper is a long and detailed explanation of the benefits of fermented foods.
This website provides a good list of foods, in a variety of categories, to help keep your colon healthy.
Keep Your Colon Healthy: Supplements
Digestive probiotics are a form of good bacteria found in the body and are essential to a healthy gut. However, not every meal will contain these probiotic rich foods, so supplementing is an important part of any digestive health strategy.
Entire books are written on options for overall colon health and colon cancer prevention. This article is not meant to be totally inclusive. While a many products could be listed here, I’m only mentioning what I have found to be KEY supplements that should be part of every GI Health program: probiotics and digestive enzymes. I have also mentioned to additional products: one for overall gut inflammation and one for gently correcting constipation.
Probiotics
Probiotics are good bacteria that support digestive health by maintaining and optimal pH in the intestinal tract. This balances out the undesirable bacteria and improves nutrient absorption. You may be incorporating probiotics into your meal and not even know it – yogurt, kefir, pickles, miso and tempeh are all probiotic powerhouses.
Adding good bacteria as a supplement goes beyond what can be obtained from food alone. I advise taking probiotics at bedtime, allowing the bacteria to populate the GI tract over night byperistalsis, without being mixed with food.
My long-time favorite probiotic is Opti-biotic, available in two sizes (60 capsules and 30 capsules) at the DrTenpenny.com supplement store. For a probiotic to be effective, it must be shelf-stable past its expiration date and precisely delivered to the intestinal tract for maximum benefit. Opti-biotic’s BioShield® technology is an innovative manufacturing process developed to ensure these two elements.
The microorganisms in Opti Biotic are protected, sealed and freeze dried away from moisture, heat, light and oxygen. This allows the bacteria to remain dormant until they are exposed to moisture in the intestinal tract. Saccharomyces boulardii is included in this formula. This is an extensively researched ‘good yeast’ that forms a lattice work in the gut for the ‘good bacteria’ to cling to. Each Opti Biotic capsule provides seven proven probiotic strains, chosen for their ability to withstand the harsh gastrointestinal environment and deliver superior results.
Opti GI Balance is another product recommended for intestinal inflammation. If you have irritable bowels symptoms (IBS), inflammatory bowel disease (IBD), chronic diarrhea or persistent small intestine cramping, adding in this supplement once a day will really help quell those symptoms. Opti GI Balance is a softgel that contains thyme oil, clove oil and oregano oil, all shown to be soothing inflamed tissues and immune-enhancing throughout the intestines. It comes as a 90-day supply and should soothe and heal your entire intestinal tract.
Constipation Issues
If you have issues with intermittent constipation, in addition to increasing exercise, water intake and eating more raw foods including apples and carrots, keeping Opti GI motility on hand is gentle way to get things moving.
Opti GI Mobility is a patented combination of ginger (Zingiber officinale) and artichoke leaf extract (Cynara cardunculus L.) delivered at a clinically proven dose to restore gastric motility, improve digestion, and relieve temporary gastric discomfort. This distinctive blend of bioactives which help to restore proper motility. In addition, it can provide relief from temporary gas, bloating and associated GI discomfort.
Digestive Enzymes
Your body naturally produces digestive enzymes to break down the food you eat. With our fast-paced and hectic schedules, we don’t always eat as cleanly as we should. Nor do we take the time to chew as thoroughly as we should, especially since adequate chewing is the first and most important step in good digestion. Including a digestive enzyme is essential for gut health.
I personally have used our digestive enzymes, Opti Digestive Support, for many years. This comprehensive blend of acid-resistant, plant-based enzymes is designed to maximize the digestion and absorption. Each capsule has enzymes to break down fat, starch, proteins, carbohydrates, fiber and difficult to digest food particles that can be associated with food sensitivities.
Opti Digestive Support includes lipase, amylase, lactase, CereCalase® and protease to aid in the digestion of protein, fat, starches, fiber and other difficult to digest foods known to cause food sensitivities. CereCalase®, a blend specially formulated to digest the cell walls of plants, providing better nutrition from a plant-based diet. Each capsule also contains gentian root, a traditional bitter herb as well as artichoke root, to stimulate production of bile and other natural enzymes.
I take 1-2 capsules after every meal. While the directions with digestive enzymes suggest taking them before eating, I’ve found they work better when taken at the end of the meal.
In Conclusion
In the 1980’s and 1990’s, most screening methods put in use were gFOBT and sigmoidoscopy. However, since the year 2000, most colon cancer screening in the United States shifted towards colonoscopy, even though its effects on reducing the incidence and mortality from colon cancer has never been proven in a solid randomized controlled trial.
Therefore, the evident question should be: has the benefit truly been worth the risk? Are there better ways to screen for risks – that then SHOULD have a colonoscopy as a confirmatory study?
Recall, an ideal screening test should be safe, readily available, convenient, inexpensive and have a high sensitivity. I think several stool and blood tests discussed in this substack that are much better for screening than an expensive, marginally safe colonoscopy which, in my opinion, should only be used to confirm a diagnosis and should NOT to be used for routine screening.
Throughout this 2-part series, I have shown that routine colonoscopies are not all they’re cracked up to be. There are several other, non-invasive screening options and many foods and supplements that should be your cornerstone to overall colon health.
While a colonoscopy is a good and important procedure for diagnostic purposes, it may be time to remove its standing as the “gold standard” of colon cancer screening.
Studies reviewed, in no particular order:
- 2002: Occult Gastrointestinal Bleeding: Detection, Interpretation, and Evaluation.
- 2009: Circulating methylated SEPT9 DNA as a biomarker for colorectal cancer
- 2011: Septin 9 methylated DNA: sensitive and specific blood test for colon cancer
- 2015: Fecal occult blood testing for colorectal cancer screening: past or future
- 2017: Colorectal cancer screening: An updated review of the available options – IMPORTANT PAPER
- 2018: Colorectal Cancer Screening—Who, How, and When?
- 2019: Fecal occult blood test in colorectal cancer screening
- 2019: Genomic Assessment of Blood-Derived Circulating Tumor DNA in Patients With Colorectal Cancers: Correlation With Tissue Sequencing, Therapeutic Response, and Survival
- 2019: mSEPT9 Blood Test (Epi proColon) for Colorectal Cancer Screening
- 2022: Source matters: a survey of cost variation for fecal immunochemical tests in primary care. (both FOBT and FIT tests cost around $6USD)
- 2022: Systematic analysis of circRNA biomarkers for diagnosis, prognosis and therapy in colorectal cancer


.png)







Comments
Post a Comment